Last September, Nora Engel, PhD, and her team joined the Coriell Institute for Medical Research to continue her work studying the differences in the risks and outcomes of cancer between people born with XX and XY sex chromosomes, traditionally biologically female or male.
Her research focuses on the disparities between the biological sexes in progression and metastasis of melanoma, but better understanding these factors for melanoma can also elucidate how our sex chromosomes may affect our risk for other forms of cancer, as well as other diseases.
Below, Dr. Engel answers questions about her work studying melanoma, why those of us with XY sex chromosomes may be more likely to develop the disease than those of us with other arrangements of sex chromosomes, and what most interests her about her work.
 |
| Nora Engel, PhD |
Nora, your lab joined the Coriell Institute for Medical Research just a few months after we launched the Camden Cancer Research Center. Can you tell me what your lab is investigating and how it is involved with the CCRC?
My lab is trying to find out why biological males (individuals with XY sex chromosomes) have a higher risk for most non-reproductive cancers (meaning all cancers except breast, ovarian, and prostate), and generally worse outcomes. We are studying melanoma as an example of sex-biased cancers, and we use mouse models for our research.
Because XX and XY individuals have different levels of sex hormones and also different sex chromosomes, our experiments are aimed at disentangling those two factors to see how they are involved in the sex disparities in melanoma.
Are there specific characteristics about that melanoma that lend it to being a good subject for investigating these differences in risk and outcome?
One thing that makes melanoma a great subject is that there are very well-established mouse models for melanoma, although until now, no one has studied the disease with the sex angle in mind.
Another reason is that it is a form of cancer that does not sicken the mice in the same way other types do. In a way, it's more humane to study if you are using an animal model.
In the mice, we are injecting XX and XY melanoma cells into biological male and female mice and comparing how fast the tumors grow, whether they generate more or less metastases, and then we compare gene expression to see differences in each of those situations.
What is known about the reasons that males tend to have higher risk for cancers and worse outcomes? Has your work with melanoma in the mouse model supported or expanded that?
There is nothing definitively known, however, one hypothesis based on the fact that XX individuals have a stronger immune response suggests that the immune systems in biological females are better at detecting and killing off cancer cells.
Another hypothesis is that the sex hormones play a role, but even though it makes logical sense, it still needs to be explored scientifically.
It’s most likely several factors all involved at the same time, and it also may relate to aging, since cancer in general is a disease of aging, and males and females age very differently.
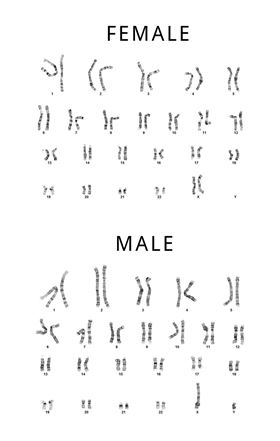 How do males and females age differently? Are the differences the result of the presence or lack of a Y chromosome?
How do males and females age differently? Are the differences the result of the presence or lack of a Y chromosome?
Possibly! There are studies showing that older males often have loss of chromosome Y. This has only been shown in blood cells, but it may be an indication that the Y protects the genome from mutations or other chromosomal aberrations. It's also possible that having two X chromosomes is helpful because even if one of them is usually inactive, they can be a backup for one another.
Aging affects different tissues and organs differently for the biological sexes (for example, those with XX chromosomes tend to experience greater muscle loss with age), but we don't yet know exactly why this is the case.
Regarding melanoma, there is an important distinction—young females (20-30) have higher melanoma risk, presumably because of high tanning salon usage; however, after that, males have higher risk overall.
We do know that the average age for presentation of melanoma is 60-65 years old, and melanomas in males have many more mutations than in females.
Using mice, you can better control those behavioral causes too I assume, keeping them out of tiny tanning salons, etc. Is maintaining behavior another benefit to the mouse model in your work?
Yes, mice don't frequent tanning salons that often! In that sense, we eliminate some of the confounding factors of sun exposure. However, if we want to, we can expose the mice to UV radiation in a controlled fashion to mimic human melanomas at sun-exposed regions.
In any case, we are also eliminating other behavioral factors that may distinguish male and female humans. However, the fact remains that the higher risk for those with XY chromosomes cannot be accounted for only because of environmental or behavioral factors because they have higher risks for these cancer, every ethnicity, culture, background, and age range. This is true even in cats and dogs!
Do you expect that what you learn about the sex differences in risk and outcome for melanoma will translate to other forms of cancer as well? Or even more broadly to other diseases? Or is it too early to tell?
I do expect our studies to inform other forms of cancer. I strongly suspect there are commonalities in the mechanisms of sex disparities, even between different cancers, although certain cancer types might have more contributions from sex-linked factors than others.
For other diseases, there may be implications: for example, if immune responses are relevant, they might also explain why 90 percent of patients treated for autoimmune disorder have XX chromosomes.
It will also be very important to study how intersex individuals are affected, because they have different numbers of sex chromosomes and that can be even more informative for how genes on the sex chromosomes contribute to differences in disease prevalence.
On the other hand, the effects of sex hormones on non-reproductive tissues (i.e., not breast, ovary, or prostate) are underexplored. We are studying how hormones interact with sex chromosomes and affect normal melanocytes. It is critical to advance knowledge of how hormones and sex chromosomes affect all normal tissues, especially to anticipate the effects of cross-hormone therapies in transgender individuals.
How could that knowledge be used to better prevent and cure, for instance, melanoma?
If we find genes that increase male risk for melanoma or produce worse outcomes, they could be used as targets for developing new therapeutic strategies. On the other hand, if we find genes that are expressed in females that somehow protect them from cancer, we could use that information to design strategies to enhance expression of those factors in males.
To you, what is most fascinating about the line of research your lab is pursuing?
I am a basic scientist and I love figuring out how different genes are expressed in different tissues and how these patterns get disrupted and rewired in cancer.
I’ve always found it fascinating that all cells have the same genes, but different genes are active in different cell types. For example, some genes active in melanocytes (the skin cells which produce melanin and are also responsible for melanoma) are different from the genes active in brain cells, or eye cells, or any other cell type.
Also, it intrigues me how an adult cell such as a melanocyte can lose its characteristics and sort of go back to a more primitive state, more similar to an embryonic cell, when it becomes cancerous.